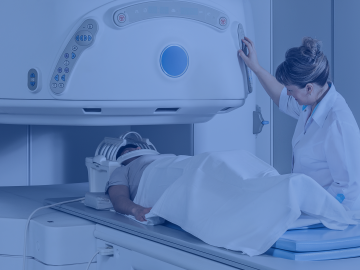
A recent article in Pharmaceutical Online on aseptic processes caught our attention, where the Parenteral Drug Association dared to ask the question, “What can be done to achieve zero particulates in parenteral manufacturing?”
The headline took us down a few veins of an important thought-exercise:
1) By presenting the query in these terms, does the PDA know something the rest of of us do not know about the prospects for such a standard?
2) Does discussion of this topic by a high-profile organization portend stricter regulations to come for PM threshold limits?
3) Is the PDA going to provide exact specifications for steps manufacturers can take to achieve zero particulates and sterility assurance?
When reading the piece in its entirely, however, none of these threads received the attention we believed they might. In fact, in the end, the author lands on the most predictable conclusion possible: detection and removal of all particulate matter is not a particularly feasible target for pharmaceutical manufacturers. (See what we did there?).
It is the causes she cites, however, that ended up being the greater surprise.
She seems to pin the core of the issue on the presence of significant variation in manufacturing processes, inspection methods (visual and subvisible), and risk assessments across the industry, and even among multiple sites within a single organization. This “lack of consistency in manufacturing processes,” she says, is what most impedes the effort.
To that, we’d argue it is not necessarily a simplified manufacturing process that will create better knowledge, awareness and protection against the presence particulate matter. Rather, it is a realized digitization of process and safety controls related to environmental monitoring, both within the facility and up and down the value chain, which can serve to materially mitigate the risk of a sterility breach, and limit damage if it occurs.
The author goes on to call out an urgent need to identify defects “at the time of manufacture,” as this can provide valuable insight about where particulates came from, and how to reduce them in the future. To us, this advice stems from a misguided assumption. Aseptic manufacturers aiming to exclude contaminants already do a pretty good job of identifying the presence of impurities. The trouble, it could be said, is they do this job too well.
Paradoxically, whenever an operator handles passive air monitoring equipment such as agar collection media, it opens the door to the possibility of needlessly wasted product, by way of false-positive contamination reports. It is unrealistic to expect a process that does not require humans to complete the job but, in an environment as critically sensitive as aseptic manufacturing, it may be time to move on from a multi-touch workflow that inherently sets the stage for frequent non-conformance alarms. (In this case, post-manufacture contamination of cleanroom monitoring equipment).
The reasons for this are clear. Every time a manufacturing run has a flagged concern, it costs a cool $16,000 just to launch an internal investigation. And the cost of sending a batch to waste that would otherwise be of good quality but for a post-production non-sterility event is $500,000.
Beyond the hard costs, any batch that gets held for investigation, whether it’s contaminated or not, goes to extend the time-to-market timeline. Anything that can be done to limit the chances of contamination during the collection process will reduce the instance of false-positives, remove an entire cost center, and allow products to be released sooner. There are simply fewer flagged batches to contend with.
Going touchless alters the workflow to reduce the number of steps human operators have to take in the course of their job that might lead to a contamination event. It’s that simple. But, how?
Tego’s entire raison d’etre is to allow progressive data to be placed directly onto physical, static assets so that industries can solve long-standing challenges. In aseptic manufacturing, the idea is for passive viable air monitoring equipment to come to life with computing power so that staff members can complete plate collection through a more streamlined procedure, which means they don’t have to touch as many of the plates, or touch them as many times.
In keeping with the PDA’s call for a more uniform approach, better internal collaboration, and open communication between manufacturers, suppliers, and regulatory agencies, touchless environmental monitoring could indeed “increase the feasibility of products being manufactured essentially free of particulate matter.” But, even if such a vision remains aspirational, reduced instance of false-positive contamination is not a bad outcome, either.
How efficient is your process of particulate-spotting?
To learn more about Tego’s touchless monitoring solutions for cGMP environments, please visit this page.
To schedule a demo of Tego’s gamma-proof technology for your aseptic facility, contact us here.